In the fast-paced world of dentistry, staying updated with the latest advancements and tools is crucial to ensure both patient satisfaction and practitioner efficiency. Tru-Tain, a renowned name in the dental industry, has recently introduced a groundbreaking innovation that promises to revolutionize the way dentists work – the KeyGuide system. In this comprehensive guide, we’ll delve deep into what the KeyGuide system is, how it works, and why it’s a game-changer for dental professionals. Whether you’re a seasoned dentist looking to upgrade your practice or a dental student eager to learn about the latest technologies, this blog post will provide you with valuable insights.
Chapter 1: Understanding the KeyGuide System
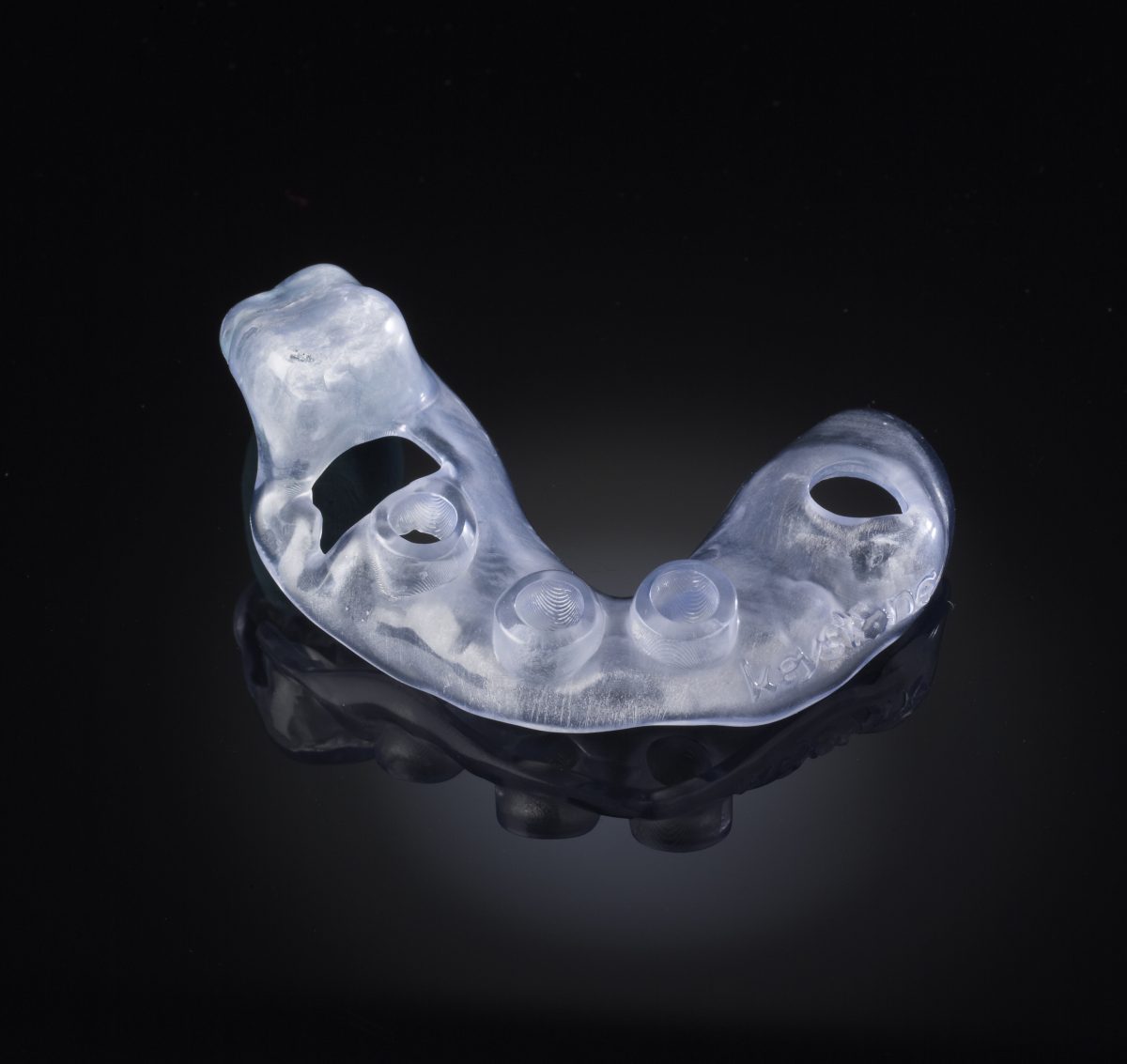
The KeyGuide system, developed by Tru-Tain, is a cutting-edge dental solution designed to enhance the precision and efficiency of various dental procedures, particularly in the realm of crown and bridge restorations. This advanced technology leverages the power of 3D printing and computer-aided design (CAD) to create highly accurate and customized surgical guides for dental practitioners.
Chapter 2: How Does the KeyGuide System Work?
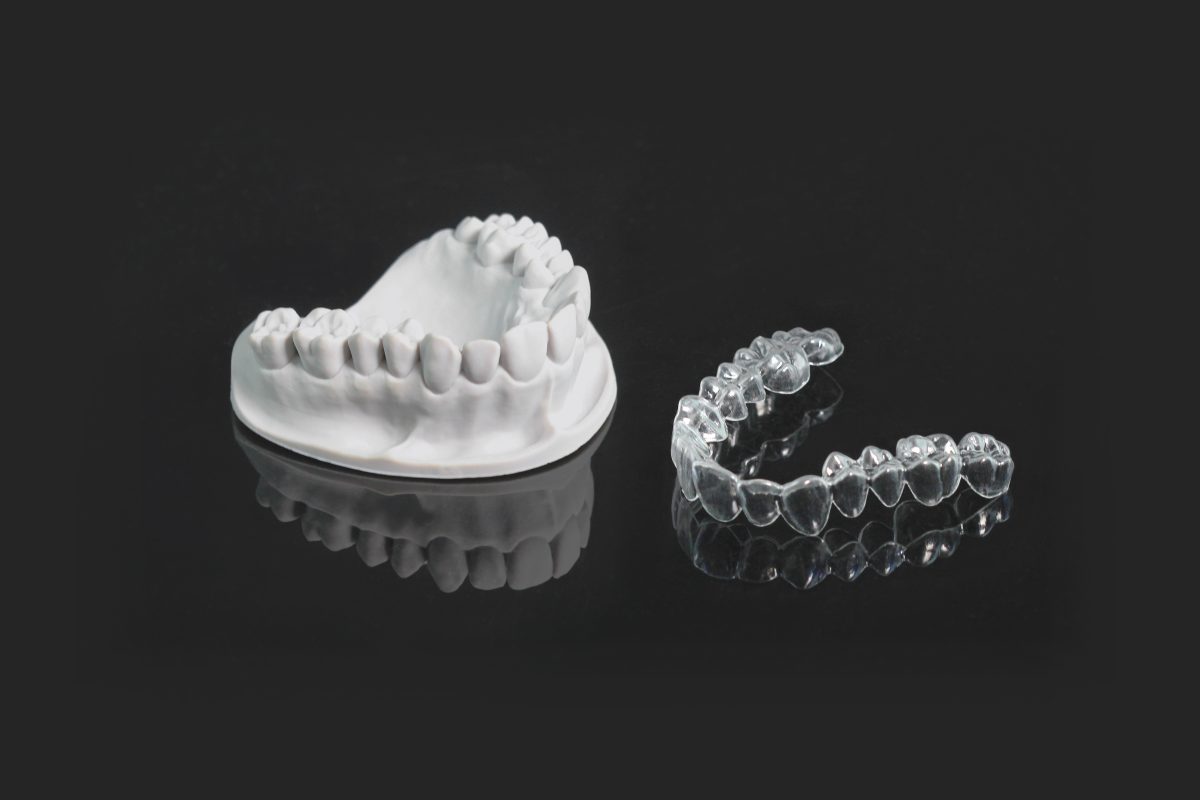
At the heart of the KeyGuide system lies its seamless integration of digital workflows. The process begins with a thorough intraoral scan of the patient’s oral cavity using advanced digital impression systems. This scan is then fed into the KeyGuide software, where the dentist can plan the placement of implants, crowns, or bridges with unparalleled accuracy.
The software utilizes the scan data to create a virtual model of the patient’s dentition, allowing the dentist to virtually “try on” various restoration options. This digital planning phase ensures optimal aesthetics, functionality, and occlusion. Once the plan is finalized, the software generates a 3D model of the surgical guide that will aid the dentist during the actual procedure.
Chapter 3: Advantages of the KeyGuide System
The KeyGuide system offers a multitude of benefits that make it a must-have tool in every modern dental practice:
- Precision and Accuracy: The system’s reliance on digital scans and CAD technology ensures that the surgical guides are tailored precisely to each patient’s unique anatomy. This results in improved clinical outcomes and reduces the margin of error.
- Time Efficiency: Traditional methods of creating surgical guides are often time-consuming and involve multiple steps. With the KeyGuide system, the entire process is streamlined, from digital planning to guide fabrication, significantly reducing chair time.
- Patient Comfort: The non-invasive nature of the digital impression process makes it more comfortable for patients, eliminating the discomfort often associated with conventional impressions.
- Enhanced Communication: The system promotes better communication between the dentist and the dental laboratory, leading to a more collaborative and efficient treatment process.
- Predictable Outcomes: Thanks to the advanced virtual planning capabilities, dentists can visualize the final result before even starting the procedure, ensuring a predictable and satisfactory outcome.
Chapter 4: Integrating KeyGuide into Your Practice
Incorporating the KeyGuide system into your dental practice requires a few essential steps:
- Invest in Training: Tru-Tain offers comprehensive training programs to familiarize dental professionals with the software and hardware components of the KeyGuide system.
- Upgrade Infrastructure: Ensure that your practice has the necessary equipment, such as intraoral scanners and 3D printers, to seamlessly integrate the system.
- Collaborate with Laboratories: Establish a strong working relationship with dental laboratories that can manufacture the surgical guides based on your digital plans.
Chapter 5: The Future of Dentistry with KeyGuide
As the dental industry continues to evolve, technology-driven solutions like the KeyGuide system are poised to reshape the way dentists approach treatment planning and execution. The potential for customization, accuracy, and time-saving offered by this system opens doors to even more innovative advancements in the field.
Tru-Tain’s KeyGuide system is a groundbreaking innovation that underscores the transformative potential of technology in dentistry. By combining 3D printing, CAD technology, and digital workflows, the KeyGuide system empowers dentists to achieve unprecedented levels of precision, efficiency, and patient satisfaction. As the dental landscape continues to evolve, embracing such innovative solutions will undoubtedly be a pivotal step towards staying at the forefront of modern dentistry.